In the world of fertility treatments, in vitro fertilization (IVF) is one of the most advanced and well-known options for couples struggling to conceive. While many people are familiar with the basic idea of IVF—where an egg is fertilized outside the body and then implanted into the uterus—the specific medical tools and tests involved in the process can be more mysterious. Among these, ultrasound and hormone testing play pivotal roles in ensuring the IVF procedure has the best chance of success.
If you’re considering IVF or are just curious about the process, you might be wondering: Why are ultrasound and hormone testing so important? How do they affect the outcome of the treatment? Let’s dive into the details.
Ultrasound in IVF: The Silent Observer
Ultrasound might sound like a high-tech medical tool, but in reality, it’s a simple and non-invasive technique that offers powerful insights into your reproductive health. During IVF treatment, ultrasound is used frequently to monitor everything from egg development to the condition of the uterus. In some cases, it’s even used to guide procedures like egg retrieval.
Monitoring Follicular Development
In a typical IVF cycle, a woman’s ovaries are stimulated with hormones to produce multiple eggs. This is a crucial part of the process because more eggs give the doctor a better chance to select healthy embryos for implantation. But how do doctors know when the eggs are ready? Ultrasound helps them track the growth and development of the ovarian follicles, which are the sacs that contain the eggs.
As the follicles grow, they should reach a certain size before they’re ready for egg retrieval. Ultrasound allows doctors to see exactly how many follicles are developing, how big they are, and if they’re growing in a healthy, consistent way. The results guide the timing of other treatments, such as the administration of a trigger shot (a final hormone injection that causes ovulation). This precision is crucial because if the eggs are retrieved too early or too late, the IVF cycle may fail.
Evaluating Uterine Health

Another key aspect of IVF is ensuring that the uterus is in optimal condition for embryo implantation. An ultrasound allows doctors to check for things like the thickness of the uterine lining and the presence of any abnormalities, such as fibroids or polyps, which could interfere with implantation. A thick, healthy uterine lining is essential because it provides a nurturing environment for the embryo to implant and grow.
Sometimes, a procedure called an endometrial biopsy or a saline infusion sonogram (SIS) is done with ultrasound to check for issues within the uterus. These procedures help rule out any potential roadblocks that might prevent a successful pregnancy.
Guiding Egg Retrieval
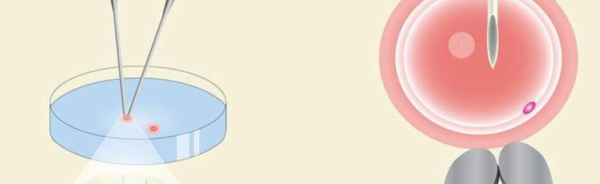
One of the most critical moments in IVF is the egg retrieval process, where mature eggs are collected from the ovaries. This procedure is typically done under sedation and is guided by ultrasound. A needle is inserted through the vaginal wall and into the ovaries to collect the eggs, and ultrasound ensures the needle is accurately placed and that the eggs are safely retrieved. Without ultrasound, this process would be much riskier and less precise.
Monitoring Ovarian Reserve
Another use of ultrasound in IVF is to evaluate a woman’s ovarian reserve—the number of eggs remaining in the ovaries. While hormone testing is often the first method for gauging ovarian reserve, ultrasound can offer a more direct look at the ovaries and give doctors an idea of how many follicles are present in each cycle. For women considering IVF at an older age or those with a history of fertility issues, understanding ovarian reserve is critical in determining the best approach for treatment.
Hormone Testing: The Body’s Internal Compass
Hormones are the body’s chemical messengers, and in the case of IVF, they’re the signals that regulate everything from egg production to the readiness of the uterus for embryo implantation. Hormone testing provides essential information about a woman’s fertility status and guides many of the medical decisions made during IVF.
Assessing Ovarian Reserve
One of the first things doctors will check when you begin IVF treatment is your ovarian reserve, which refers to the number and quality of eggs remaining in your ovaries. The more eggs you have, the better your chances of success in IVF, as more eggs increase the likelihood of producing viable embryos.
To assess ovarian reserve, doctors typically test levels of two hormones:
- Follicle-Stimulating Hormone (FSH): FSH is responsible for stimulating the ovaries to produce eggs. Elevated FSH levels can be a sign that your ovaries are starting to lose their ability to respond to hormonal stimulation, which is a common sign of aging.
- Anti-Müllerian Hormone (AMH): AMH is a hormone produced by the follicles in the ovaries. A higher AMH level typically indicates a better ovarian reserve. Low AMH can suggest a reduced number of eggs.
These hormone levels provide a snapshot of your fertility potential. If your ovarian reserve is lower than expected for your age, it might suggest that IVF will be more challenging, and your doctor may adjust your treatment plan accordingly.
Tracking Ovulation
Once your IVF cycle begins, hormone testing becomes essential to track your body’s response to stimulation. During IVF, doctors administer hormones like Human Chorionic Gonadotropin (hCG) to trigger ovulation once the eggs have reached maturity. This timing is incredibly important: ovulation needs to happen at exactly the right time to ensure that the eggs are retrieved when they are most viable.
Doctors often measure estrogen levels during this phase as well. Estrogen levels should rise as the follicles develop, so tracking estrogen helps doctors gauge how well your body is responding to the ovarian stimulation and whether adjustments to your medication are necessary.
Monitoring Luteal Phase and Pregnancy
After egg retrieval, the luteal phase begins, and hormones like progesterone become critical. Progesterone helps prepare the uterine lining for embryo implantation. If progesterone levels are insufficient, your doctor may supplement with progesterone injections or vaginal suppositories. Hormone testing during this phase ensures that your body is ready for embryo transfer.
After the embryo is transferred, hormone tests (usually measuring hCG) help determine whether implantation has occurred and if the pregnancy is progressing. A rising hCG level is a strong indicator of pregnancy, and continued testing helps monitor the health of the pregnancy during the early stages.
How Ultrasound and Hormone Testing Work Together
While ultrasound and hormone testing are incredibly powerful on their own, together they form a comprehensive picture of your reproductive health during IVF. Hormone tests provide the biochemical data, while ultrasound provides the visual confirmation. Both tools allow doctors to adjust your treatment in real-time, fine-tuning everything from medication dosages to timing, in order to maximize your chances of a successful outcome.
For instance, if hormone testing reveals that estrogen levels aren’t rising as expected, ultrasound can provide a visual assessment of the follicles and help the doctor decide whether to adjust the dosage of medication. Conversely, if ultrasound shows that follicles aren’t developing properly, hormone levels can help explain why and guide treatment decisions.
Why These Tests Matter
In short, ultrasound and hormone testing are not just routine procedures in IVF—they are foundational to ensuring that each step of the process is as effective as possible. IVF is a delicate and complex procedure, and every small detail counts. These tests help doctors make critical decisions that could mean the difference between success and failure.
The reality is that IVF can be a long, expensive, and emotionally taxing journey, and the role of ultrasound and hormone testing can’t be overstated. They give doctors the ability to adjust treatments based on your specific needs, and they help reduce the risks associated with IVF, offering a better chance of achieving a healthy pregnancy.
Conclusion
If you’re embarking on an IVF journey, understanding the importance of these tests will help you feel more confident and informed as you move through the process. Ultrasound and hormone testing may sound intimidating, but they are crucial tools that provide insights into your body’s readiness for IVF and help your doctor tailor your treatment to give you the best possible chance of success. Ultimately, they are your partners in ensuring that the IVF process is as smooth and effective as possible.
So, the next time you hear the term “ultrasound” or “hormone testing,” remember that these aren’t just standard procedures—they are your roadmap through the complex world of IVF, guiding you toward your goal of becoming a parent.